Pregnant Nana (Not her real name) is rushed to the Maternity Unit of the 37 Military Hospital in labour. She is a National Health Insurance Scheme (NHIS) subscriber, meaning she did not have to pay for anything under the Free Maternal Healthcare policy but what turned up was a total cash-and-carry affair as she paid for covered services before being provided the needed healthcare upon arrival at the hospital.
Nana and her husband, a farmworker, lacked the finances to pay for the bills so every bill given to them was followed by phone calls to relatives and friends to beg for money.
After spending over GHc3,000.00 already on bills, the couple is hit with the tragic news: their newborn could not survive.
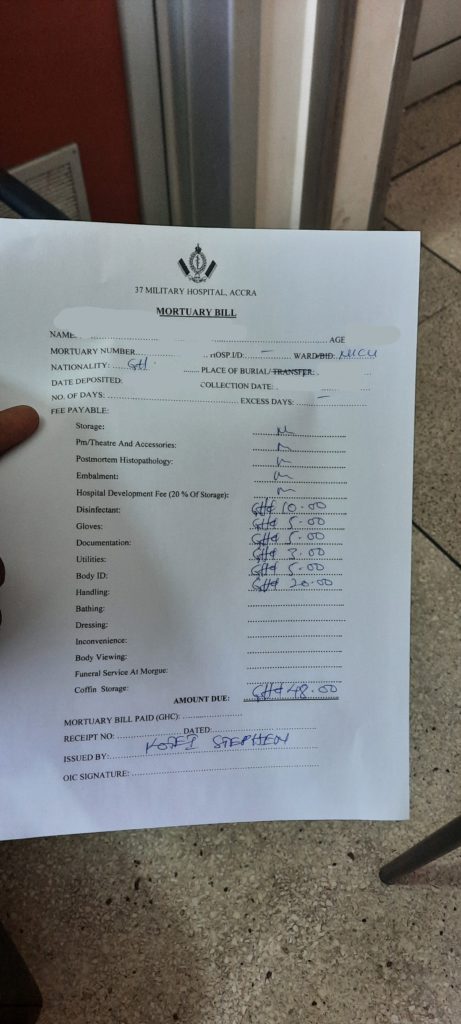
As if that was not enough, the grieving parents were then hit with another news of the body being detained till a GHc1,067.14 being the cost of staying in the Neonatal Intensive Care Unit (NICU) prior to the death, is completely cleared, before a death certificate and clearance would be issued for the release of the corpse.

The NICU bill was not the end of their trauma, an additional bill awaited them at the mortuary. While they grieved their loss, they were, again, confronted with where to find the financial help to settle the NICU and mortuary bills. The compounded bad news left the couple numb.
Mrs Addo-Cobbiah, Deputy Chief Executive, Operations, National Health Insurance Authority (NHIA), described this situation as totally wrong and unlawful.

Corruption Watch contacted the 37 Military Hospital for comments but as at the time of filing this report they had not granted an interview six weeks after submitting a request for an interview
Nana’s case is just one of several ordeals pregnant women and their partners go through in our government hospitals despite being covered by NHIS. Corruption Watch investigator, Francisca Enchill goes undercover, to expose the agony of pregnant women in hospitals, a spectacle of pregnant women being confronted with the option of paying cash before accessing the otherwise free healthcare under the Free Maternal Healthcare policy or refuse to pay and die.
This is in spite of the existence of the NHIS that states clearly that Maternal Healthcare (MHC) is absolutely free, including even abortion complications.
Corruption Watch uncovered this Pay or Die phenomenon in investigations conducted at the 37 Military Hospital, Mamprobi Hospital, popularly known as Mamprobi Polyclinic and Maamobi General Hospital, popularly known as Maamobi Polyclinic.
Findings
The investigation found gross abuse of the purpose for the introduction of the Free Maternal Healthcare Policy. It was found that health facilities have set their own rules to extort money from pregnant women during Antenatal, Delivery and Postnatal care.
Some of these illegal payments that put unnecessary impediments on access to maternal healthcare have somehow been made official, hence, pregnant women are directed to make payment at the bank. The investigation also found that health workers charge and directly take payments without issuing receipt for charges which are supposed to be free.
Our investigation established that Free Maternal Healthcare (FMHC) is currently only ‘on paper’ but practically, it is non-existent in all the facilities captured in this investigation although hospitals make claims for services rendered under free maternal healthcare and those claims are paid for by the NHIS.
Tertiary Hospitals
Although the NHIS policy pays higher claims to the referral hospitals than those paid to the Polyclinics and general hospitals, it was established that at the referral hospitals, pregnant women are unlawfully charged higher amounts for the same services provided by the Polyclinics.
Dr Chris Opoku Fofie, Head of Safe Motherhood Program at the Family Health Division of the GHS, said all health facilities under the GHS run scans for free.

However, this investigation established a contrary fact. Many pregnant women were unaware of their entitlement under the FMHC policy. It also found that even when pregnant women, who were aware of their entitlement, put it to health workers and demand their entitlement, they denied it flatly that antenatal services are free.
37 Military Hospital

At the 37 Military Hospital, pregnant women are denied the benefit of free scan. A scan costs Ghc100.00 at this facility.
37 Military Hospital: It was discovered that the list of laboratory tests given to pregnant women cost Ghc250 at the laboratory of 37 Military Hospital. Other tests like Full Blood Count cost Ghc35.
Corruption Watch contacted the 37 Military Hospital for comments but as at the time of filing this report they had not granted an interview six weeks after submitting a request for an interview
Emergency admission – 37 Military Hospital
Pregnant women, who develop complications during the course of pregnancy at the 37 Military Hospital, are made to pay for every drug, lab tests and scans on a cash-and-carry basis. What is more, if pregnant women are detained for further medical observation, they are charged Ghc60 as admission fee for each day spent under medical observation.
Despite having paid for every service already, during discharge, the bill is above Ghc1,000.00 and can increase depending on the number of days spent on admission.
Delivery
The delivery day is the most anxious day in the nine-month-journey of a pregnant woman. Not every pregnant woman that enters the delivery room is lucky to make it alive. Not every baby makes it out alive and not every baby who is born safely survives the first few days. Hence, the moment labor starts, it is all prayer for families for the safety of mother and child.
This stage is, however, a bumper revenue collection day for health facilities as they issue killer bills with no empathy. Partners or sometimes friends and family are traumatized with the guilt of failing to make timely payments for drugs and tests.
Women, who are not able to pay their bills, are detained until the amount is raised by their family or a philanthropist.
37 Military Hospital: Delivery at the 37 Military hospital makes no room for the poor. The Maternity Unit of this hospital is run like a private health facility, with comparatively, very high charges. Every single medication, materials or service needed for delivery is purchased by patients and their families on a cash-and-carry basis.
It was also found that despite having a pharmacy inside the Maternity Unit where medicine could be dispensed when needed, pregnant women are asked to buy medical supply even when its need is not yet required, sometimes leading to some women returning home with unused medical supplies like infusion when they are discharged from the hospital.
Despite being made to buy everything and pay for every service in a cash-and-carry manner, the medical bill issued to patients during discharge is very high with the lowest being above Ghc1,000.
Although the FMHC policy requires hospitals to submit all bills as claims to the NHIS without billing the patient any amount directly, 37 Military Hospital does the contrary. They bill pregnant women for even admission and consultation at the Maternity Unit. Meanwhile, poor people referred to this hospital visit the facility hoping to depend on their FMHC entitlements.
According to the FMHC policy, NHIS covers the bill 100%, hence does not cover part of the bill for pregnant woman to pay for the other half. However, 37 Military Hospital practices the contrary. The bill they issue claims NHIS only covers a portion of the bill and the patient pays the rest.
37 Military Hospital issues bills ranging from Ghc800-Ghc1,000 for women who have Spontaneous Vaginal Delivery. This amount goes higher depending on the number of days the patient spends on admission as GHc60 is added automatically each day as admission fee. Out of this amount, the hospital’s bill states that NHIS covers GHc159.70 and the patient pays the rest.
The NHIS described this as unlawful.
Caesarean Section(CS): 37 Military Hospital charges between GHc2,000 to Ghc5,000 for Caesarean Section. The longer you stay under medical observation, the higher the bill. According to information on the bill issued at the hospital, NHIS covers only GHc543.20 of the total bill.
Postnatal
The periodic postnatal care, commonly referred to as Weighing, is relatively completely free at the 37 Military Hospital. However, Neonatal Intensive Care Unit (NICU) service, is not free.
At the 37 Military Hospital, newborns are charged a daily admission fee of Ghc50. The number of days spent in the NICU determines the magnitude of the bill given to parents.
At the 37 Military Hospital, babies who spend up to three days in the NICU, are billed Ghc 1,064.17. According to the information on the bill of the hospital, NHIS covers GHc565.74 of the total cost, while the family pays the rest.
This amount has an automatic GHc50 increment for each additional day spent at the NICU.
Mamprobi Hospital
This was the only hospital amongst those we investigated that required pregnant women to spend up to GH¢96.00 even before being accepted to register for antenatal service.
As part of the registration expenses, nurses at the Mamprobi Hospital were also found directing pregnant women on their first visit to their welfare shop to purchase a mandatory package. This mandatory package contained some items needed only on the delivery day but pregnant women were made to buy them at GH¢26.00 even before being registered and given their maternal health record book to begin antenatal.
This package is given to the Welfare Shop by the nurses to be sold to pregnant women.
Dr. Charlotte Cato, Specialist in charge of Mamprobi Hospital, denied that the facility makes any demand before allowing pregnant women to access antenatal care. However, Corruption Watch’s investigation found this claim by Dr. Cato to be false.
Scan: The Mamprobi Hospital, officially charges pregnant women GH¢35.00 for a scan. This payment is made as many times as a scan is required.

One other financially draining unique policy of the facility was that scans done in facilities outside the Mamprobi Hospital were not accepted by the health workers. Pregnant women, who run scans before visiting the facility to avoid the queue, are made to pay for a new scan even if the first scan done outside was done the same day.
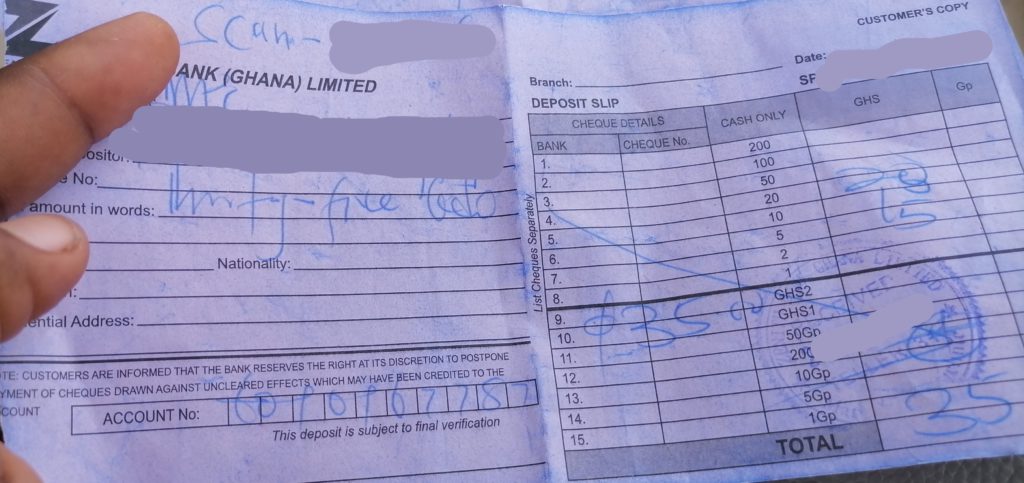

Despite establishing that Mamprobi Hospital charges NHIS holders GH¢35.00 for scan, Dr. Charlotte Cato, the Specialist in charge of the hospital, denied the charges. According to her, the facility only charge pregnant women who do not have NHIS cover GH¢30.00 but it is at no cost for NHIS subscribers.
Laboratory test
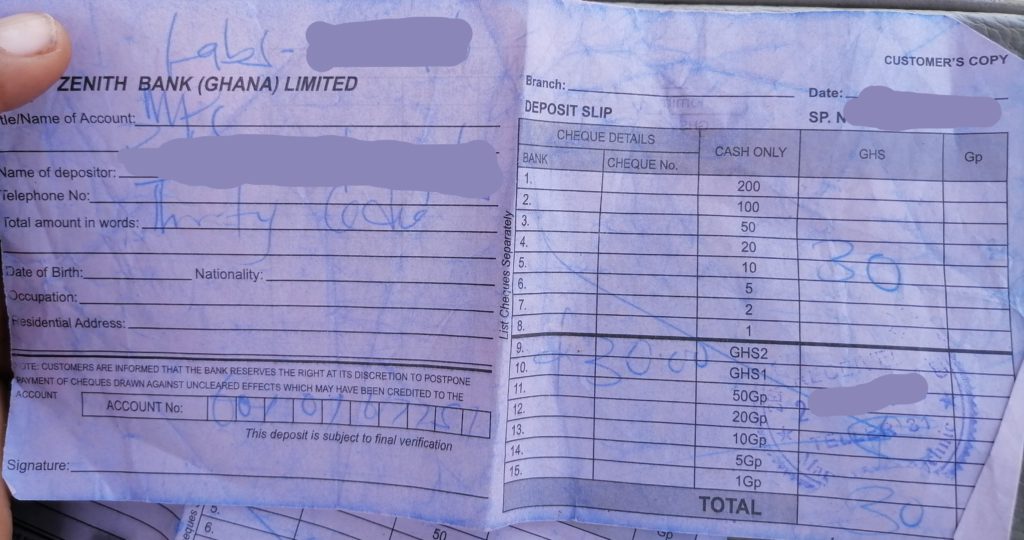
At the Mamprobi hospital, pregnant women are denied access to free laboratory tests as well, the first group tests are divided into two. First half cost each pregnant woman Ghc30. The other half of the test costs Ghc20 for NHIS holders. Meanwhile, all these tests are covered under the FMHC policy.
Management response
According to the Head of the hospital, Dr. Charlotte Cato, these tests are covered by NHIS in her facility so pregnant women enjoy them for free, but Corruption Watch’s independent investigation established that the hospital charges for these tests.
Mamprobi Hospital: At this facility, antenatal drugs are free. The drugs are actually already packaged with a stationed staff right at the antenatal unit disbursing them. Vitamin C was, however, paid for.
Maamobi General Hospital
At the Maamobi General Hospital, pregnant women were charged GH¢10.00 at the consultation room on a first visit. This, the nurses claimed covers service delivery and some medical supplies.
Scan: At this facility, pregnant women were officially charged GH¢ 40 for a scan. This amount is paid as many times as a scan is required.
Management response
Edem Datsomor, Principal Nursing Officer of the Maamobi General Hospital, who refused to grant a video or audio interview said, scan was not part of the FMHC entitlement in their hospital.
Mrs. Vivian Addo-Cobbiah, Deputy Chief Executive, Operations at NHIA, said NHIA pays for scans through the claims.
Laboratory tests: Dr Chris Fofie said that facilities are operating according to the rules governing the FMHC policy by offering pregnant women a completely free laboratory service.

However, this investigation established that laboratory tests are not free for pregnant women in any of the facilities investigated.
At the Maamobi General Hospital, the first main laboratory tests costs Ghc50. Other tests done in the course of pregnancy were equally not free.
During another test at this hospital, the laboratory technician took the request form, took the samples for the test and charged Ghc35 and received payment directly from the pregnant woman inside the lab without issuing receipt.
Response of Management
Edem Datsomor, the Principal Nursing Officer of the facility, on behalf of the facility, said the amount paid by NHIS as antenatal cover per visit is not enough to cover laboratory tests although their supervising institution, GHS supports NHIA’s insistence that this service is free.
She, however, said the hospital does not permit the collection of direct payment by staff for any service delivered apart from the bank, hence, any staff caught doing that will be taken through disciplinary process for punitive action to be applied.
Drugs: At this hospital, the drugs that are available are paid for and pregnant women are referred to buy the rest from private pharmacies on the grounds of unavailability.
Delivery: Drugs, scans and lab test during delivery, including blood are paid for on a Cash-and-carry basis. Also, parts of the charges for delivery by CS were Ward fee, CS procedure, Suture, discharge, among others, costing around GHc 1,200 as official charges of the hospital, that are accompanied by official receipt aside extra cost incurred from drugs and tests requested by the hospital, which are run in private facilities outside the hospital.
NHIS described this as unlawful and unfair as well.
Postnatal

Maamobi General Hospital offers NICU services to newborns. Although this service is supposed to be free, the service is not enjoyed for free.

At the Maamobi General Hospital, NHIS covered pregnant women are required to make payment of Ghc200 or more as NICU deposit. Aside this, drugs, lab tests and RBS test are all run on a Cash- and-carry basis. NICU expenses alone can cost a parent over Ghc500 at the Maamobi General Hospital.

NHIS described this practice also as unlawful and gave a breakdown of what the practice should be.
Mrs Vivian Addo-Cobbiah, Deputy Chief Executive, Operations at NHIA said facility heads claiming ignorance about the benefit are not being sincere.
STAKEHOLDER MEETINGS
This investigation established that although all the health facilities submit their claims to NHIS for payment, pregnant women are charged for every free service rendered at their facilities.
Pregnant women are expected to budget up to Ghc500 for antenatal expenses in normal pregnancy and about Ghc2,000 or more for antenatal expenses during pregnancy complications.
Mrs Vivian Addo-Cobbiah, Deputy Chief Executive, Operations at the NHIA, described these as barriers that prevent the poor from accessing antenatal care, defeating the purpose for which the policy was introduced.
NHIS response to Laboratory tests
According to Mrs. Addo-Cobbiah, Deputy Chief Executive, Operations, NHIA, all laboratory tests required in the cause of pregnancy are all fully covered by the NHIS, hence, pregnant women should not pay any amount of money for that service.
DRUGS
Although pregnant women are entitled to free antenatal drugs, some hospitals charge for the drugs, some claim unavailability of some drugs and direct patients to buy them outside and some prescribe drugs that are not on the list of NHIS drugs, hence requiring patients to pay to get the drugs.
Postnatal
The NHIS cover of a mother also covers the postnatal cost of a newborn. This cover includes any care given to the baby right after birth if admitted at the Neonatal Intensive Care Unit (NICU) and the normal postnatal visits/weighing till the baby is three months old. At three months, the baby then needs his/her own separate NHIS cover.
SDG Goal 3

SDG goal 3.1 targets the reduction of the global maternal mortality ratio to less than 70 per 100,000 live births by 2030.
3.2 It further aims to end preventable deaths of newborns and children under five years of age, with all countries aiming to reduce neonatal mortality to at least as low as 12 per 1,000 live births and under-five mortalities to at least as low as 25 per 1,000 live births.
According to the 2019 UN Inter-Agency Group for Child Mortality Estimation, the infant mortality rate of Ghana is 34 deaths per 1,000 live births and Ghana’s maternal mortality rate is currently 308 per 100,000 live births, According to the GHS.
Although the infant and maternal mortality rate has been declining since the introduction of the Free Maternal Healthcare policy, the margin of decline hasn’t been different from the margin of decline in the years before the introduction of the policy.
For Ghana to meet the SDG goal 3 target, the policy formulators, as well as those at the point of service delivery, must ensure that the Free Maternal Healthcare policy is made to work fully to remove barriers and expand access to maternal healthcare.
Watch full video here:
Francisca Enchill’s report.
Watch out for part II in our next edition for more shocking revelations in other hospitals.

