The Ghana Health Service (GHS) has confirmed that positive monkeypox cases have increased to 18.
Speaking at a Covid-19 briefing on Wednesday in Accra, the Director of GHS, Patrick Kuma-Aboagye, said out of 72 suspected cases that were sampled as of June 14, 2022, 18 have been confirmed positive.
“The last case was a week ago, so that is where we are as far as monkeypox is concerned,” he said.
He added that “let’s not make it appear as if monkeypox had just appeared in Ghana. We can’t have a disease that spreads to the countries to your left and right, and then the virus jumps over you. But now that we are actively searching, we are finding them, which is good because it means we can stop the spread.”
According to him, infected people range in age from nine months to 41 years. However, no deaths have been reported as a result of the virus.
The majority of the cases, he said, have been reported in Greater Accra, Ashanti, Bono, and the Eastern Regions.
Meanwhile, the Director-General of the World Health Organisation, Tedros Adhanom Ghebreyesus, has announced he would convene an emergency committee meeting on Thursday, June 23 to assess the implication of the outbreak of the monkeypox virus.
He said the committee will be tasked to determine “whether this outbreak represents a public health emergency of international concern.”
Mr Ghebreyesus explained that the decision to convene the committee meeting is also due to a recent “unusual” behaviour shown by the virus as it keeps spreading in countries beyond Africa.
About monkeypox
Monkeypox is endemic in countries such as Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Ghana, Ivory Coast, Liberia, Nigeria, the Republic of the Congo, Sierra Leone, and South Sudan.
Transmission of virus
Transmission occurs primarily via droplet of respiratory particles usually requiring prolonged face-to-face contact, which puts household members of active cases at greater risk of infection.
Transmission can also occur by inoculation or via the placenta (congenital monkeypox). There is no evidence, to date, that person-to-person transmission alone can sustain monkeypox infections in the human population.
Secondary, or human-to-human transmission can result from close contact with infected respiratory tract secretions, skin lesions (open wounds/injuries) of an infected person or objects recently contaminated by patient fluids or lesion materials.
Symptoms
The infection can be divided into two periods:
The invasion period (0-5 days) characterised by fever, intense headache, lymphadenopathy (swelling of the lymph node), back pain, myalgia (muscle ache) and an intense asthenia (lack of energy).
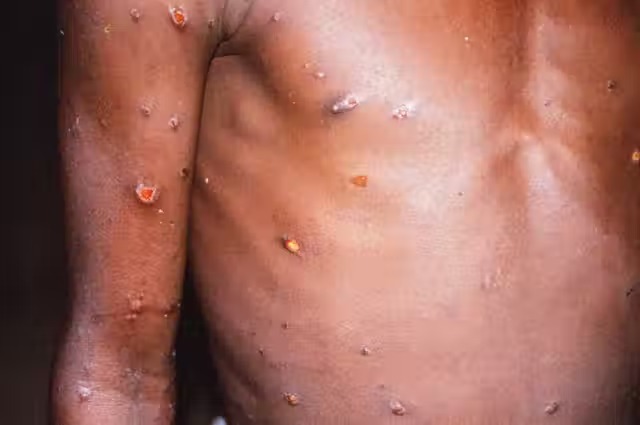
The skin eruption period (within 1-3 days after the appearance of fever) where the various stages of the rash appears, often beginning on the face and then spreading elsewhere on the body.
The face (in 95% of cases), and palms of the hands and soles of the feet (75%) are most affected.
Treatment/Vaccine
There are no specific treatments or vaccines available for monkeypox infection, but outbreaks can be controlled.
Vaccination against smallpox has been proven to be 85% effective in preventing monkeypox in the past but the vaccine is no longer available to the general public after it was discontinued following global smallpox eradication.
Prevention
In the absence of specific treatment or vaccine, the only way to reduce infection in people is by raising awareness of the risk factors and educating people about the measures they can take to reduce exposure to the virus.
Regular hand washing should be carried out after caring for or visiting sick people.
Reducing the risk of animal-to-human transmission. Efforts to prevent transmission in endemic regions should focus on thoroughly cooking all animal products (blood, meat) before eating.
Public health educational messages via the media – broadcast, electronic and social – is highly advised.
Healthcare workers and those treating or exposed to patients with monkeypox or their samples should consider being immunized against smallpox via their national health authorities.